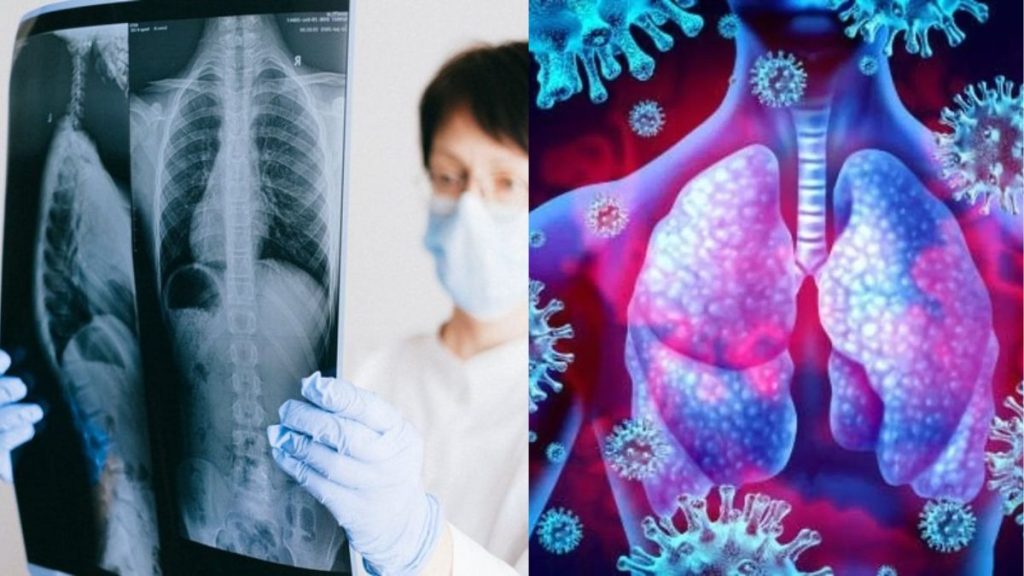
Respiratory infections like influenza or COVID-19, cause stress on cells and organs. They result in acute respiratory distress syndrome (ARDS). It can eventually lead to death in the elderly or fragile people.
Professor Johan Auwerx at EPFL’s School of Life Sciences said, “Novel therapeutic strategies to address ARDS, instead of fighting the infectious agent, could try to elicit the tolerance of the host organism towards the inflammatory challenge by boosting its natural adaptive stress responses.”
 In a new study, EPFL’s Adrien Mottis and his colleagues show that such a strategy can exploit a biological phenomenon known as “mitohormesis”. Mitohormesis describes the fact that mild stress on a cell’s mitochondria can trigger a number of reactions that actually increase cell health and function.
In a new study, EPFL’s Adrien Mottis and his colleagues show that such a strategy can exploit a biological phenomenon known as “mitohormesis”. Mitohormesis describes the fact that mild stress on a cell’s mitochondria can trigger a number of reactions that actually increase cell health and function.
We know that the main energy-harvesting organelles of the cell are Mitochondria. They are constantly monitored by the cell’s “surveillance” system. This continuous quality control can activate adaptive compensatory responses when mitochondria are defective or subjected to stress. It is known as the ‘mitochondrial stress responses’.
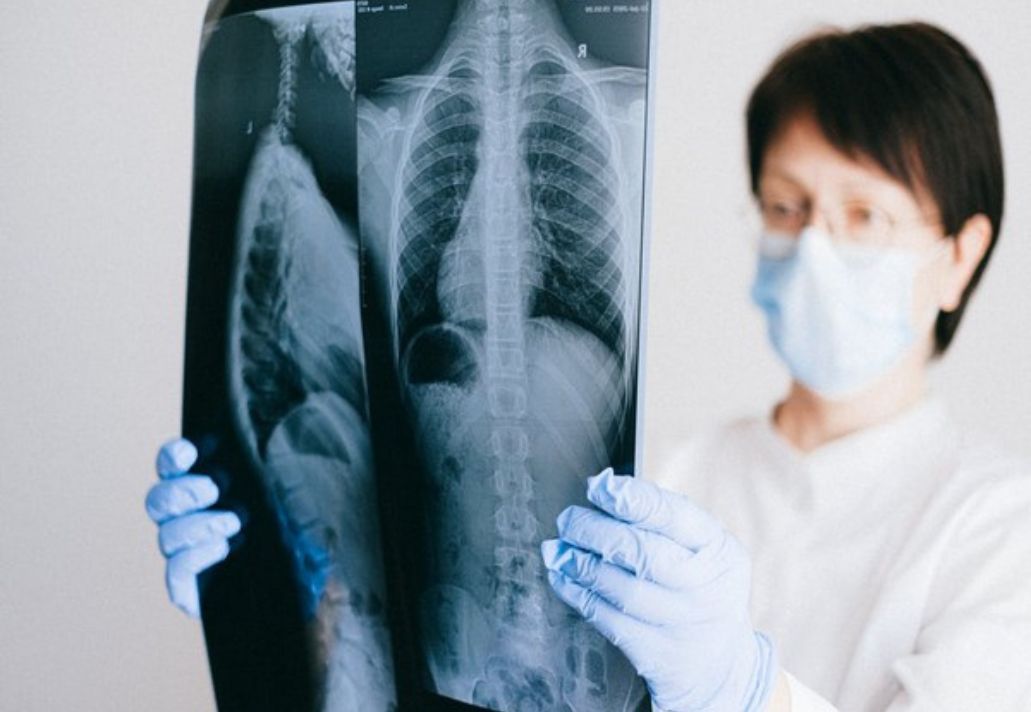 Mottis who led the study, said, “A mild level of mitochondrial stress can therefore be beneficial overall for the cell and the organism since the positive effect of these stress responses can overcome the negative effect of the initial stressor.”
Mottis who led the study, said, “A mild level of mitochondrial stress can therefore be beneficial overall for the cell and the organism since the positive effect of these stress responses can overcome the negative effect of the initial stressor.”
The researchers screened 52 selected novel molecules, such as tetracycline and 9-test-butyldeoxycycline (9-TB), which are potent enough to trigger mitohormesis at low doses, although they have no antibiotic effect – that is, they don’t bother. The microbiome of the host. In their tests on mice, the compounds induced mild mitochondrial stress and beneficial mitohormetic responses that increased the animals’ tolerance to infection by influenza virus. Lastly, the authors said, “These findings open innovative therapeutic avenues by targeting mitochondria and mitohormesis to fight inflammatory challenges and infections.”